Contact dermatitis develops into a rash of itchy, red skin 1. Red patches that resemble a burn may be visible on your ankles. A warm sensation and swelling is often present after the ankles come in contact with a substance. The skin on your ankles may blister, ooze and have a dry crust-like appearance. Oct 06, 2017 Extract fresh aloe gel from your garden or borrow from a neighbor. Apply a tablespoon of aloe vera paste on your affected skin. Allow it to dry for few hours. Hydrating property housed in this ingredient will soften your thick skin on the ankle bone.
Medically reviewed by Drugs.com. Last updated on May 8, 2019.
- Health Guide
What Is It?
Hyperkeratosis is a thickening of the outer layer of the skin. This outer layer contains a tough, protective protein called keratin.
This skin thickening is often part of the skin's normal protection against rubbing, pressure and other forms of local irritation. It causes calluses and corns on hands and feet. It can cause whitish areas inside the mouth.
Other forms of hyperkeratosis can occur as part of the skin's defense against:
- Chronic (long-lasting) inflammation
- Infection
- Radiation of sunlight
- Irritating chemicals
Less often, hyperkeratosis develops on skin that has not been irritated. These types of hyperkeratosis may be part of an inherited condition. They may begin soon after birth and can affect skin on large areas of the body.
There are many examples of hyperkeratosis. They include:
- Corns and calluses. Corns and calluses develop in areas of skin exposed to repeated friction or pressure. In response, thick layers of dead skin cells pile up and harden.Corns usually develop on irritated toes. Calluses form on the soles of the feet and the palms of the hands.For many people, corns and calluses are simply a cosmetic nuisance. But for others, they are a painful and troublesome medical problem.
- Warts. Warts are small bumps on the skin that are caused by human papilloma virus (HPV) infection. Plantar warts grow on the soles of the feet.HPV usually is spread by direct contact. It is typically spread by touching or shaking hands with someone who already has a wart. It may also be spread by coming in contact with a contaminated surface. For example, by walking barefoot on a gym floor or a pool deck or by wearing someone else's shoes.
- Chronic eczema. Eczema is an inflammation of the skin. It can be triggered by allergies, irritating chemicals and other factors. Eczema is also called dermatitis.Eczema causes itching, redness and tiny blisters. When the inflammation is difficult to control, chronic eczema can lead to:
- Hyperkeratosis
- Dry skin
- Scaling
- Changes in skin color
- Localized hair loss
- Lichen planus. This condition may appear as a lacy white patch on the inside of the mouth. Or it may be an itchy, violet, scaly patch elsewhere on the skin. Lichen planus may be related to an abnormal reaction of the immune system.
- Actinic keratoses. These are flat, red, rough, sandpaper-like spots or patches of skin. They can be as tiny as a few millimeters.They are caused by excessive exposure to the ultraviolet radiation of sunlight. They occur on sun-exposed areas of skin. And they have the potential to develop into skin cancer.
- Seborrheic keratoses. These are small, noncancerous skin growths. They can be tan, brown or black. They appear on the face, trunk, arms or legs. Seborrheic hyperkeratoses are very common. Their cause is a mystery.
- Inherited conditions. Several inherited conditions cause hyperkeratosis. They cause a widespread, thick, platelike scaling of the skin. Symptoms begin either shortly after birth or during early childhood.
Symptoms
Many forms of hyperkeratosis are painless. However, corns, calluses and plantar warts can cause a great deal of discomfort.
Diagnosis
Depending on your specific pattern of skin symptoms, your doctor will ask whether you:
- Have a family history of skin problems
- Have a personal history of allergies
- Have frequent sun exposure
- Use dentures or orthodontic dental appliances
- Unconsciously chew on your cheek or tongue
- Use smokeless tobacco
Sometimes, your doctor can diagnose the cause of your hyperkeratosis based on your history and symptoms and by examining your skin. This often is the case with corns, calluses, warts and chronic eczema.
If you have chronic eczema that could be allergy-related, the doctor may suggest allergy testing.
In some cases, a biopsy may be taken to confirm the diagnosis. In a biopsy, a small piece of tissue is removed to be examined in a laboratory. If your doctor suspects actinic keratoses, you may need to have a skin biopsy to confirm the diagnosis and to rule out skin cancer.
If your child develops many areas of hyperkeratosis, your doctor may review your family history and skin symptoms. This will help to determine if your child has an inherited disorder.
Expected Duration
How long a particular form of hyperkeratosis lasts depends on its cause. For example, corns and calluses usually last as long as a person continues to wear poorly fitting shoes. Warts may disappear on their own. But this may take several months.
Once they develop, actinic keratoses or seborrheic keratoses are long-term conditions. They do not disappear without treatment.
Inherited forms of hyperkeratosis are lifelong conditions.
Prevention
Some forms of hyperkeratosis are very easy to prevent:
- Corns and calluses. Wear comfortable shoes.
- Plantar warts. Avoid going barefoot in gyms, locker rooms or pool areas.
- Chronic eczema. Avoid potential triggers to help to limit or prevent eczema symptoms. For example, avoid:
- Extreme temperatures
- Dry air
- Harsh soaps
- Bubble baths
- Irritating chemicals
Also, try using blankets and clothing made of cotton. Fabrics such as wool, silk and rough synthetics can be more irritating. Avoiding or removing triggers for your allergies also may help.Get advice and treatment for mild eczema to help prevent it from becoming a long-lasting condition (chronic eczema). - Actinic keratoses. Limit your sun exposure to early morning or late afternoon hours. Wear protective clothing and a hat when you go outdoors. Apply sunscreen to exposed areas with a sun protection factor (SPF) of a least 30.
Treatment
The treatment of hyperkeratosis depends on the type and possible cause.
- Corns and calluses. Use moleskin or padding next to the affected area to decrease pain. Always wear proper footwear to avoid further friction.
Don't shave away or cut a corn or callus on your own. Consult a health professional for advice and treatment.
- Warts. A health care professional can remove warts. This is done by one of the following:
- Freezing them with liquid nitrogen (cryosurgery)
- Vaporizing them with a laser
- Trimming them away surgically
If the treatment does not reach the layer of skin infected with the virus, the wart can come back in the same place. Repeat treatments may be necessary.
Warts can be treated at home with nonprescription remedies. Self-treatment will take longer for the wart to go away compared to treatment in a medical setting. Self-treatment may be more effective after you have been treated by a health care professional. This is especially true if a wart appears to be large or deep.
If you have diabetes or poor circulation, you should always be treated by a health care professional. This will help you to avoid injury and infection.
- Chronic eczema. Your doctor usually will prescribe a corticosteroid ointment or cream. Moisturizing the skin is also very important.
- Lichen planus. Like chronic eczema, lichen planus usually is treated with corticosteroid ointment or creams.
- Actinic keratoses. Your doctor may use cryosurgery to remove a single actinic keratosis. Multiple keratoses can be treated with skin peels, laser therapy or dermabrasion.
- Seborrheic keratoses. This can be removed with cryosurgery or with a scalpel.
- Inherited conditions. There is no cure for these conditions. To treat large areas of scaly skin, your doctor may suggest rubbing special emollients into the skin.
When To Call a Professional
Make an appointment to see a health care professional or podiatrist if:
- You have painful corns or calluses
- You develop a painful thickening on your foot that looks like a plantar wart
People with diabetes should have their feet examined regularly by a health professional to avoid skin infections from corns, calluses or warts.
Adults should examine their skin regularly after age 20. This is particularly true for those who have a history of working or playing for long hours in the sun. If you are not sure how to examine your skin, ask your doctor for guidance.
If you think you have hyperkeratosis or eczema, schedule an appointment with a health care professional.
Whenever you notice that a skin growth or mole has changed color, size or shape, call your doctor for a more urgent appointment. Any new mole or other growth should be checked for signs of cancer.
If you have actinic keratoses, call your doctor for treatment.
Prognosis
Most forms of hyperkeratosis are local skin problems that have a good prognosis.
Actinic keratoses can develop into squamous cell skin cancer.
External resources
American Academy of Dermatology
P.O. Box 4014
Schaumburg, IL 60168-4014
Phone: 847-330-0230
Toll-Free: 1-888-462-3376
Fax: 847-330-0050
http://www.aad.org/
P.O. Box 4014
Schaumburg, IL 60168-4014
Phone: 847-330-0230
Toll-Free: 1-888-462-3376
Fax: 847-330-0050
http://www.aad.org/
American Podiatric Medical Association (APMA)
9312 Old Georgetown Road
Bethesda, MD 20814
Phone: 301-571-9200
Toll-Free: 1-800-275-2762
Fax: 301-530-2752
http://www.apma.org/
9312 Old Georgetown Road
Bethesda, MD 20814
Phone: 301-571-9200
Toll-Free: 1-800-275-2762
Fax: 301-530-2752
http://www.apma.org/
National Cancer Institute (NCI)
U.S. National Institutes of Health
Public Inquiries Office
Building 31, Room 10A03
31 Center Drive, MSC 8322
Bethesda, MD 20892-2580
Phone: 301-435-3848
Toll-Free: 1-800-422-6237
TTY: 1-800-332-8615
http://www.nci.nih.gov/
U.S. National Institutes of Health
Public Inquiries Office
Building 31, Room 10A03
31 Center Drive, MSC 8322
Bethesda, MD 20892-2580
Phone: 301-435-3848
Toll-Free: 1-800-422-6237
TTY: 1-800-332-8615
http://www.nci.nih.gov/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
Published online 2011 Sep 22. doi: 10.4081/dr.2011.e24
PMID: 25386276
Abstract
Many people living in developing countries still prefer to sit on the carpet or uncarpeted floor, and many times they sit in a cross legged position. Continuous rubbing and friction of the ankles over the carpet or the plain hard surface may cause callosity of the ankles. This can cause a cosmetic problem. We describe a case series of ankle hyperkeratosis referred to our outpatient clinic in Ahwaz in the south west of Iran from 2005–2010. These patients had localized hyperkeratosis on two ankles or the front of ankles. This article aims to help the clinician become more familiar with the morphological characteristic of this problem which may occur in people of Eastern origin.
Key words: ankles, hyperkeratosis, callosity, crossed legs, habit.
Introduction
Callosity is a plaque of hyperkeratosis caused by repeated friction and/or pressure. A corn is a sharply demarcated callosity occurring over a bony prominence. This is usually on the hand or foot and is painful. Repeated friction or trauma on the extensor surfaces, such as elbows, knees and also ankles, cause hyperkeratosis., People living in developing countries still have the habit of sitting in a cross legged position on a plain, hard surface, rather than using furniture. Ankle callosity and hyperkeratosis is a common finding among subjects with this habit and these cause a cosmetic problem. We describe a case series of ankle hyperkeratosis among people with the habit of sitting cross legged.
Case Report
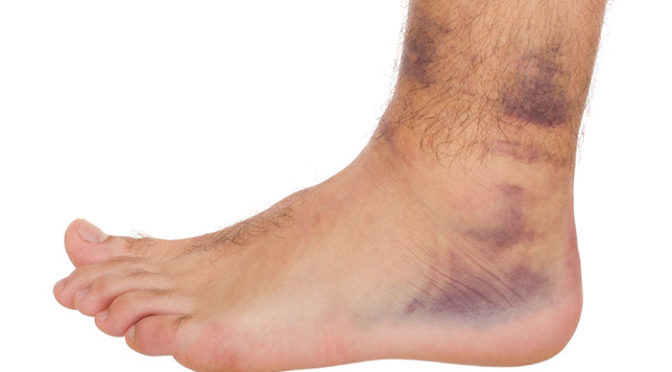
The case series consisted of 148 cases (112 women and 36 men) with a mean age of 32 years (age range 18–57 years old) referred to our private clinic and Imam Hospital, Ahwaz, in the south west of Iran from 2005 to 2010. All cases had the habit of sitting cross legged on the carpet or uncarpeted hard surface and not on the furniture. In this position, their lateral ankles touched the carpet or the plain, hard surface. This bilateral contact resulted in repetitive minor trauma directly associated with the patients' habit of sitting cross legged. There were no other symptoms. Patients were referred for cosmetic reasons and almost none of the patients knew the cause. Some of the patients, while praying, touched the carpet with their knees, the back of the feet and one side of the external ankle. Clinical examination showed localized hyperkeratosis. This was well defined and of a dark color with minimal scaling on the external ankles or on the front of the ankles (Figures 1–4). Table 1 shows the number of cases in each age group; the condition is most common in the 31–40 year old age group.
Ankle hyperkeratosis (callosity). (Photograph courtesy of Dr M Omidian.)
Localized hyperkeratosis (callosity) in the front of the ankle. (Photograph courtesy of Dr M Omidian.)
Table 1
| Age years | N. patients |
|---|---|
| 0-20 | 8 |
| 21-30 | 10 |
| 31-40 | 57 |
| 41-50 | 41 |
| 51-60 | 18 |
| 61-70 | 14 |
Cross legged position. (Photograph courtesy of Dr M Omidian.)

Ankle hyperkeratosis on the ankle and the lower front of the ankle (callosity). (Photograph courtesy of Dr M Omidian.)
Discussion
Many people, especially non-Westerners, who usually sit on a plain, hard surface in a cross legged position, or who sit on their knees, may develop callosities on prominent areas of their bodies, such as their ankles or dorsa-lateral aspects of their feet. The knees may also be involved. These conditions develop as a result of continuous and repeated friction of the prominent areas. They are usually associated with hypermelanosis, and roughening of the lesions and their surroundings.– In this case series, we report 148 cases over a period of five years who asked for treatment for cosmetic reasons. This shows that the condition is frequently seen and can be a cosmetic concern. Some general physicians and almost all the patients are not informed about its etiology. Our cases showed asymptomatic localized hyperkeratosis on the ankles due to chronic pressure and friction. Both frictional stress and family history may play a role in the pathogenesis of this condition. Hyperkeratosis usually takes some years to develop and is a result of repeated trauma to the skin from friction and pressure. In our series, there was no evidence of hereditary disorders, such as keratoderma or systemic factors producing the hyperkeratosis. It is believed to be due to chronic mechanical stimulation of the ankles. The characteristic yoga sitting position on plain, hard floors exerts mechanical stress because of repeated and prolonged pressure. Calluses and corns on the feet are usually the result of deformity sometimes associated with dynamic damage to foot function. They are made worse or even caused by unsuitable footwear and are usually painful., The cases in our series did not have any symptoms, and limb formation and function was normal. The condition could not be related to footwear but patients had a habit of sitting with one foot tucked under their body or in a cross legged position. These cases did not have any history or clinical feature of psoriasis or eczema. Hyperkeratosis is a normal protective response of the skin. It becomes pathological when the callus or corn grows so large that it becomes the source of symptoms. On the back of the foot, factors provoking callosities include footwear and a habit of sitting with the foot tucked under the body with or without a prominent underlying talus., It is most common in the 31–40 year old age group because the condition is progressive. It starts in childhood and after many years the callus or the corn becomes thicker. The condition was more common in women than men, because in our geographical area most of the women are housewives who work at home and sit on the carpet.
In conclusion, clinicians dealing with patients who have the habit of sitting cross legged should consider the importance of ankle callosity for a differential diagnosis from psoriasis, eczema and keratoderma.
References
1. Singh D, Bentley G, Trevino SC. Callosities, corn and calluses. BMJ. 1996;312:1403–6.[PMC free article] [PubMed] [Google Scholar]
2. Denise B, Freeman DPM. Corn and cal-luses from mechanical hyperkeratosis. Am Fam Physician. 2002;65:2277–80. [PubMed] [Google Scholar]
3. Krishnamurthy S, Sigdel S, Brodell RT. Frictional asymptomatic darkening of the extensor surfaces. Cutis. 2005;75:349–55. [PubMed] [Google Scholar]
4. Wahlberg JE. Occupational hyperkeratosis in carpet installers. Am J Ind Med. 1985;8:351–3. [PubMed] [Google Scholar]
5. Verma SB, Wollina U. Callosities of cross legged sitting: Yoga sign-an under-recognized cultural cutaneous presentation. Inter J Dermatol. 2008;47:121–4. [PubMed] [Google Scholar]
6. Dishan S, George B, Saul GT. Callosities, corn, and calluses. BMJ. 1996;312:1403–6.[PMC free article] [PubMed] [Google Scholar]
7. Cox NH, Finaly AY. Crossed-Leg callosities. Acta Derm Venereol. 1985;65:559–61. [PubMed] [Google Scholar]
8. Verbov JL, Monk CJE. Talar callosity: a Lttle-recognised common entity. Clin Exp Dermatol. 1991;16:118–20. [PubMed] [Google Scholar]
Articles from Dermatology Reports are provided here courtesy of PAGEPress
